You’re probably awash in ‘forever chemicals.’ Here’s why that matters
There’s a high chance PFAS are in your food, water and blood
Lori Youmshajekian • January 30, 2023

Scientists estimate more than 200 million Americans are drinking PFAS-contaminated tap water. [Credit: Pexels | Creative Commons]
A vast and pervasive group of synthetic chemicals known as PFAS – short for per- and polyfluoroalkyl substances – lurk in many things you might use every day: nonstick pans, cosmetics, waterproof clothes, and even some dental floss and guitar strings. A growing body of evidence is showing these compounds pose significant health risks. Yet many people don’t even know what PFAS are, let alone why they should be concerned and how they can reduce their personal exposure. Here’s what you need to know.
What are PFAS?
Per- and polyfluoroalkyl substances are compounds that have a long string of carbon atoms punctuated by fluorine atoms. The bonds between the two elements are “some of the strongest bonds that we can observe,” says Kimberly Garrett, a postdoctoral research associate in environmental toxicology at Northeastern University. “They don’t occur a lot in nature and they’re very, very hard to break.”
These heavy-duty carbon-fluorine bonds are the reason why PFAS are often called “forever chemicals.” They are extremely resistant to breaking down naturally in the environment – both by enzymes in soil and water and in our bodies. Instead, they leave our bodies gradually through urine, menstrual blood or breastmilk, according to the U.S. Centers for Disease Control and Prevention.
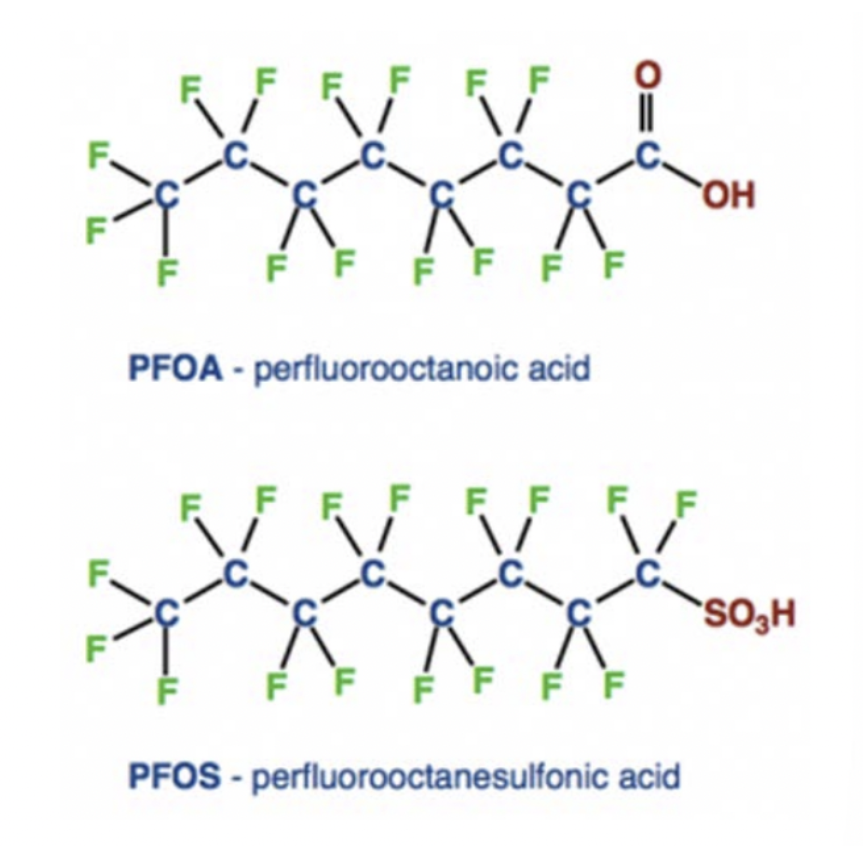
PFOA and PFOS, two common PFAS compounds, owe their longevity to the strong carbon-fluorine bonds characteristic of PFAS. [Credit: U.S. Environmental Protection Agency | Public Domain]
Some PFAS can linger in the body for up to eight years. They are so persistent that they’re likely to exist in the blood of almost everyone in the US, including newborns. And they are even more stubborn in the environment, with some taking more than 1,000 years to degrade.
The same properties that make them so tenacious in the environment also make them incredibly useful to us. “They’re very resistant to chemical degradation, environmental degradation,” Garrett says. “That makes them really useful for a lot of industrial applications and even things in our day-to-day lives.”
And they pop up in places you might not expect — like microwave popcorn. Think back to the last time you made this tasty movie-night snack: The reason why the oil stays trapped in the bag is probably because of a PFAS-based coating. In fact, one study linked people who ate more popcorn with higher concentrations of PFAS in their blood.
Their oil- and water-repellent properties mean PFAS are likely a sneaky add-on to dozens of other things you might encounter day to day: fast-food packaging, raincoats and some electronics.
There might be as many as 9,000 distinct types of these compounds hidden in our surroundings, and scientists have investigated only a handful of them. “There are thousands of these things,” says Joseph Braun, an epidemiologist at Brown University. “We actually don’t know what the heck people are exposed to.”
While everyday items are how most people are exposed to PFAS, much higher concentrations are found in areas where the compound leaches from industrial manufacturing facilities into waterways, including the Cape Fear river in North Carolina.
They can also make their way into the air or into groundwater at airports and military bases from the PFAS-laced firefighting foam used at those facilities. A U.S. government analysis of 10 communities near current or former military bases found that residents’ PFAS levels in blood were up to nine times the national average.
“It’s one of the most important environmental contamination stories of our time,” says Northeastern’s Garrett.
The substances have been found in the most remote corners of the globe, even in wild fish in the Arctic. One study put a number on just how many Americans swallow the tasteless toxins from drinking water: more than 200 million, the authors estimate, or about 60% of the country.
“These things get transported around the environment and they bioaccumulate, so they move up the food chain,” Braun says.
So, how bad are they?
Some of the health effects of certain PFAS have been known for decades. Chemicals company DuPont de Nemours Inc., one of the biggest manufacturers of PFAS chemicals in the world, knew of PFAS’ toxicity as far back as 1965 when a company-funded study found that the livers and kidneys of rats got heavier after exposure.
Then, workers started getting sick. A 1979 survey of employees at DuPont’s West Virginia Teflon plant found a potential link between PFAS exposure and liver damage. A later internal study found elevated levels of kidney and mouth cancer in workers at the same facility.
“They had internal knowledge of the health effects of exposure to these chemicals at an industrial level,” Garrett says. “However, they kept that information private.”
What followed was a prolonged and complex legal battle that exposed the internal studies about the health effects of PFAS. It also led to one of the largest cohort studies ever conducted in the U.S., investigating PFAS levels and health effects in about 70,000 people who may have been exposed.
The groundbreaking study concluded that there was a probable link between C8 – also known as PFOA, a PFAS compound widely used in nonstick cookware and stain resistant carpet – and testicular cancer, kidney cancer, high cholesterol, thyroid disease and ulcerative colitis.
Dozens of studies since then have confirmed those associations. Studies also found new correlations with PFAS exposure: weaker immune responses to vaccines and lower birth weights.
The Environmental Protection Agency recently set a new health advisory level for PFOA in drinking water: 0.004 parts per trillion. That’s significantly stricter than its previous limit of 70 parts per trillion. An analysis conducted by the Environmental Working Group, an advocacy organization, found that PFAS levels in water far exceeded the previous advisory level in many major U.S. cities, including Miami, New Orleans and Philadelphia, and posits that no more than 1 part per trillion is safe for human consumption
Even though that amount recommended by the EPA may sound infinitesimally small, our bodies find it difficult to flush out some longer-chain PFAS because the stronger bonds make them more prone to accumulating in our blood through prolonged exposure.
Because several studies have found them so harmful, two types of PFAS – PFOA and PFOS – were phased out in the U.S. in the early 2000s. PFOA was the main substance used to produce Teflon for many years, and PFOS was the main ingredient in Scotchgard, a widely used stain repellant.
“These are referred to as legacy PFAS,” says Jamie DeWitt, a toxicologist at East Carolina University. But because of their persistence in water, soil and crops, “the exposure is still ongoing,” she says.
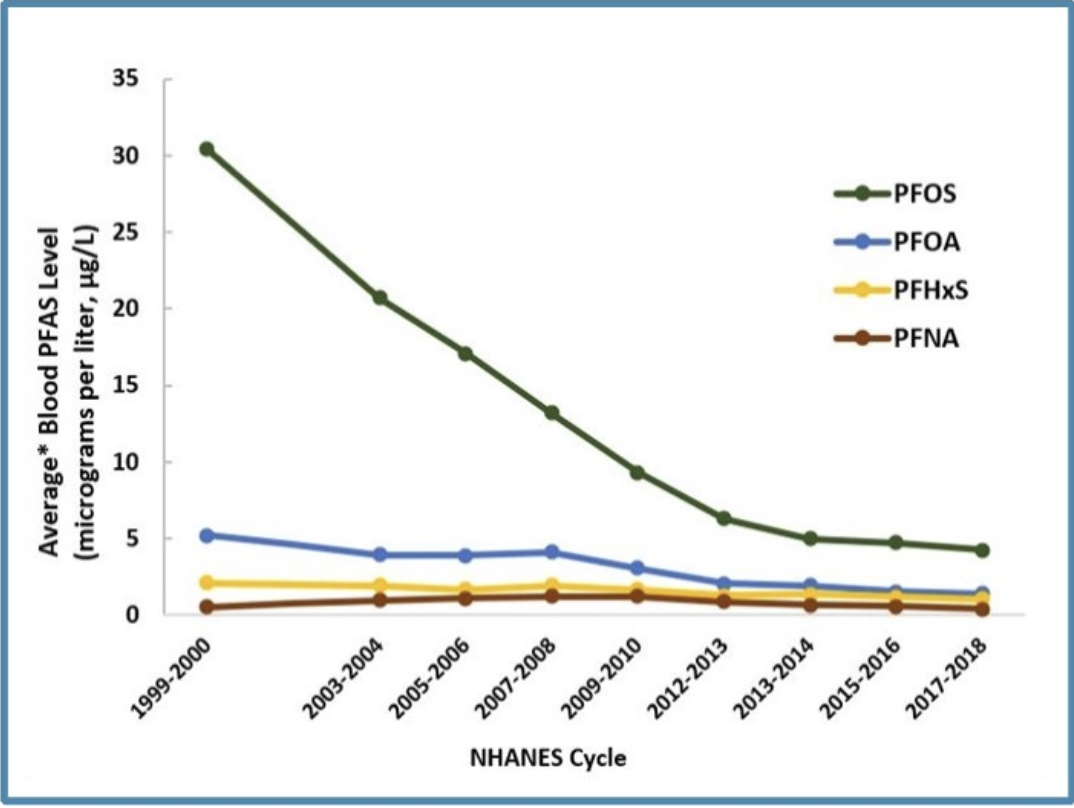
The levels of legacy PFAS in Americans’ blood have declined since they were phased out of production in the U.S., according to the National Health and Nutrition Examination Survey, a nationwide program that assesses the health, nutrition and environmental exposures of U.S. adults and children. [Credit: Centers for Disease Control and Prevention | Public Domain]
There’s a next generation of PFAS. Are they less dangerous?
Now, researchers are playing Whac-A-Mole with second-generation PFAS created to replace the phased-out compounds.
In 2009, DuPont (now rebranded as The Chemours Company) introduced a PFOA replacement labeled HFPO-DA, otherwise referred to as its patented name, Gen X. With similar stain- and water-resistant properties, it’s found in food packaging, nonstick coatings and firefighting foam.
“They’ve replaced them,” says Braun. “They found something that looks really similar to [the phased-out PFAS] and does the same job.” Scientists and epidemiologists like Braun know little about how to measure these new compounds, he says, so they’re “playing catch up.”
Gen X and other PFAS replacements have shorter carbon-fluorine chains, which means they might not last as long in our blood, according to studies performed on mice and rats. But some researchers remain wary.
“There’s a lot of rhetoric from chemical manufacturers saying that these short-chain replacement PFAS are safer,” Garrett says. “There’s really still a lot of evidence to suggest that they are similarly impactful both on the environment and on human health. They may get through your body faster, but they still last in the environment.”
In mice and rats, Gen X was flushed out of their systems anywhere from a few hours to a few days. “It’s still a sufficient amount of time for chemicals to produce adverse health outcomes in the body, especially if exposure is ongoing,” DeWitt says.
But a spokesperson for Chemours, the company behind the production and use of Gen X, minimized the risk. “HFPO-DA does not pose human health or environmental risks when used for its intended purpose – industrial manufacturing processes,” spokesperson Cassie Olszewski said in an email.
A huge hurdle for researching these health effects is that they take time to appear.
“The diseases that they produce are latent,” DeWitt explains. “They may take years before they show up in population studies… just because they don’t hurt people immediately doesn’t mean that they aren’t hazardous.”
What can we do about it?
Unless you’re directly exposed through your workplace – like a military base that may have used PFAS-containing firefighting foam, or a place manufacturing the products containing them – food is probably your main exposure to PFAS, says Braun, the Brown University epidemiologist.
“For most of us, it’s diet,” he says. “They end up in a lot of food products either from packaging or processing of the foods, as well as contaminants in our food supply. They also have been in drinking water, and so we can get exposure from there.”
Braun recommends a balanced diet to hedge your exposure. “We don’t really know what the major food sources are,” he says, adding it’s probably best to favor a diet with fewer packaged and processed foods. The Food and Drug Administration echoes his advice, recommending a “varied and well-balanced diet” for food safety.
Other suggestions from Braun: Installing a tap water filter and a vacuum cleaner with a HEPA filter to “capture all the icky stuff that’s coming out of the exhaust,” adding that PFAS can linger in dust.
“We don’t have any effective ways to get rid of them once they’re in us,” he says. “So really preventing exposure is important.”
That’s easier said than done, though. Buying unprocessed foods and water filters may be too expensive for some consumers, Braun notes.
“It’s a white rich-person problem to have the luxury to worry about this,” he says. “For some of the poor neighborhoods or marginalized communities in our country, chemical exposures are not bubbling up to their top ten worries… but that doesn’t mean it’s not a problem and someone shouldn’t help them.”
East Carolina University’s DeWitt suggests clueing into where your exposures might come from. She recommends perusing the Green Science Policy Institute and the Silent Spring Institute websites to get informed and make savvy purchasing decisions. The Skin Deep database is also helpful for consumers trying to avoid PFAS-containing cosmetics, Braun says. And an interactive map created by the Environmental Working Group tracks known sites of PFAS contamination.
But Braun believes that consumers shouldn’t have to manage their chemical exposure risks. “It’s not the individual’s responsibility to do those things,” he says. “That’s what regulations are supposed to do, they’re supposed to protect us from those things.”
Last year, eight federal agencies — including the FDA and the Department of Defense — announced plans to address the PFAS problem. Their plans include adhering to the EPA’s PFAS advisory limit of 0.004 parts per trillion; conducting cleanup assessments at Department of Defense sites around the country; and testing the food supply for potential contamination.
But, as DeWitt explains, the standards set at the federal level are toothless. “The advisory that EPA has issued for PFAS are not enforceable,” she says. “They’re their recommendations.”
States, however, have been “very proactive” at taking measures to limit their citizens’ exposure to PFAS, DeWitt says.
Earlier this year, California adopted laws to ban PFAS in cosmetics and textiles and to require more robust reporting on products that contain the compounds. “California is such a big market that it’s likely to have downstream effects that will impact people in other states,” says Northeastern’s Garrett.
Maine went a few steps further, banning intentionally added PFAS in all new products after 2030, except where it is essential to health and safety or where there is no alternative.
“If it falls under the definition of PFAS, it should be regulated as a PFAS chemical,” she says. “We need to eliminate nonessential uses of those PFAS chemicals, so ‘essential’ being things that if the PFAS were not there, the product would endanger someone’s life.”
But the regulation for PFAS is still nascent. Garret believes the U.S. needs to step up on regulating PFAS-heavy firefighting foams and should work on an enforceable federal standard for PFAS in drinking water.
“I don’t believe that there’s any government or regulatory agency that is going far enough to regulate PFAS chemicals in a way that’s comprehensively protective of human health and the environment,” Garrett says.
“There is momentum,” Braun adds. “We need to keep in mind that just because it’s not our problem anymore in the United States, it could be someone else’s problem.”