Could you lose your leg because of a tampon?
The biology behind the rare “tampon disease,” toxic shock syndrome
Lucy Hicks • March 9, 2018
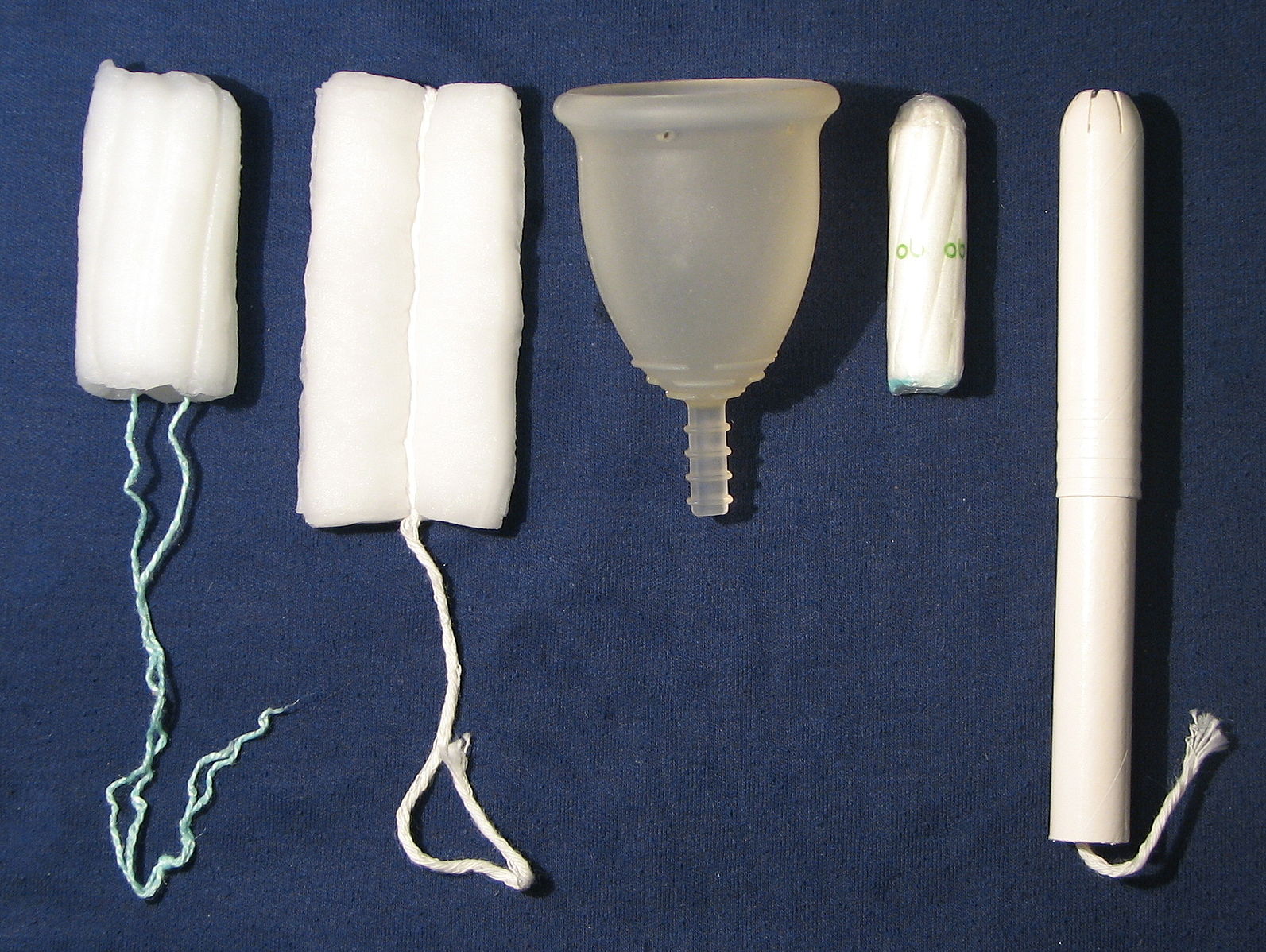
Super-absorbent tampons increased the risk of toxic syndrome in the early 1980s. How common is it now? [Image Credit: Wikimedia Commons]
Toxic shock syndrome (TSS) is a rare but serious condition that periodically finds its way into the headlines — most recently with Lauren Wasser, a model who lost her right leg to TSS in 2012, and recently had part of her left leg amputated due to lasting effects of the condition. TSS is primarily associated with tampons, but it can actually happen to anyone with an open wound where bacteria can infiltrate.
Potent toxins produced by two common strains of bacteria, staphylococcus aureus or streptococcus pyogenes, can trigger TSS; though staph is the usually the culprit in menstrual-related cases. It may sound scary, but these microbes naturally live on our skin, inside our noses, and throughout our throat and lungs. Researchers have also found them in the vaginas of healthy, menstruating women.
Before you read on, don’t freak out — the vagina has lots of naturally occurring bacteria that help prevent infection. It’s an ideal environment for bacteria: warm, with lots of moisture and nutrient-rich blood for bacteria to snack on. Add in a surface for them to colonize, such as a tampon or menstrual cup, and you’ve got the perfect breeding ground. When a tampon is left in for an extended period (beyond the recommended four to eight hours), it allows for more bacterial colonization. If that bacteria happens to be staph, at high concentrations it can release the toxin TSST-1 into the bloodstream.
Our bodies generally have strong defenses against invading pathogens. There are markers on these pathogens, called antigens, that our immune systems recognize. T-cells, a type of white blood cell, bind to the antigens, and trigger an immune response to prevent the foreign invader from causing further infection. Think of an antigen as a key to a locked door. Only a specific antigen can “unlock” the specialized cells designed to neutralize a certain threat; the body releases tailored signaling proteins, known as cytokines, which recruit the body’s cells to carry out this response.
TSST-1 is an especially dangerous toxin because it uses this defense system against us. Known as a superantigen, TSST-1 can override the body’s specific antigen to T-cell reactions. TSST-1 acts almost like a skeleton key; it can “unlock” many different immune responses. To give you an idea of scale, the typical antigen calls approximately 0.01 percent of the body’s immune cells into action; superantigens like TSST-1 can activate up to 20 percent of immune cells. (That’s 2000 times more cells than normal!)
Unleashing that many immune cells results in a system overload, known as a cytokine storm, which causes the symptoms of shock commonly associated with TSS: high fever (102 degrees), drop in blood pressure, rash, flaking or peeling skin, vomiting, and diarrhea. Without immediate medical attention, TSS can result in multi-organ failure and gangrene, as was the case with Lauren Wasser.
While this condition is scary and horrible, it is exceedingly rare; in 2016, the CDC reported just 323 cases, of which just 174 — 54 percent — were women. (Unfortunately, the CDC doesn’t share whether the cases were menstrual-related on not.) Additionally, roughly 95 percent of staph TSS cases are non-fatal, and can cause less damage if you catch the signs early.
So while you probably want to avoid getting toxic shock syndrome, just remember that the condition is rare. Just follow the instructions on the tampon box, and you should be fine.
3 Comments
Even though it is rare, this information is frightening and horrible … thank you for sharing your gratifying information.
And that’s why you don’t leave tampons and/or menstrual cups in for longer than 8 hours.
I wonder if in the demands of the modeling world she wasn’t given breaks that would allow her time to change her tampons.
My menstrual flow was so heavy that I would need to change a tampon in far less than eight hours. My sleep was even interrupted with the need to change it.